The World Health Organization (WHO) on August 14, 2024, declared a global health emergency for mpox (formally monkey pox) due to the surge in mpox in the Democratic Republic of Congo (DRC) and other countries in Africa. It is a now a “public health emergency of international concern,” (PHEIC).
The surge is due to spread of a new mutation (clade I) that appears to spread quickly from person to person and is more deadly. It was initially reported in Africa, but one case has now been reported outside of the African continent in Sweden.
Why is mpox spreading faster?
Mpox is a virus and is part of the pox family (Poxviridae) like smallpox and spreading quickly due to the type of mutation worsened by close living conditions and increase person to person skin contact with infected body fluids. The average age of person infected in DRC is 22 years of age and affects both men and women but also is reported in children. It is transmitted through sexual contact and person to person skin contact.
The risk of death with the mutation is up to 11 % compared to less than 4 % with the mpox strain (clade II) found outside of Africa and worldwide.
Why is the new mpox more deadly or dangerous?
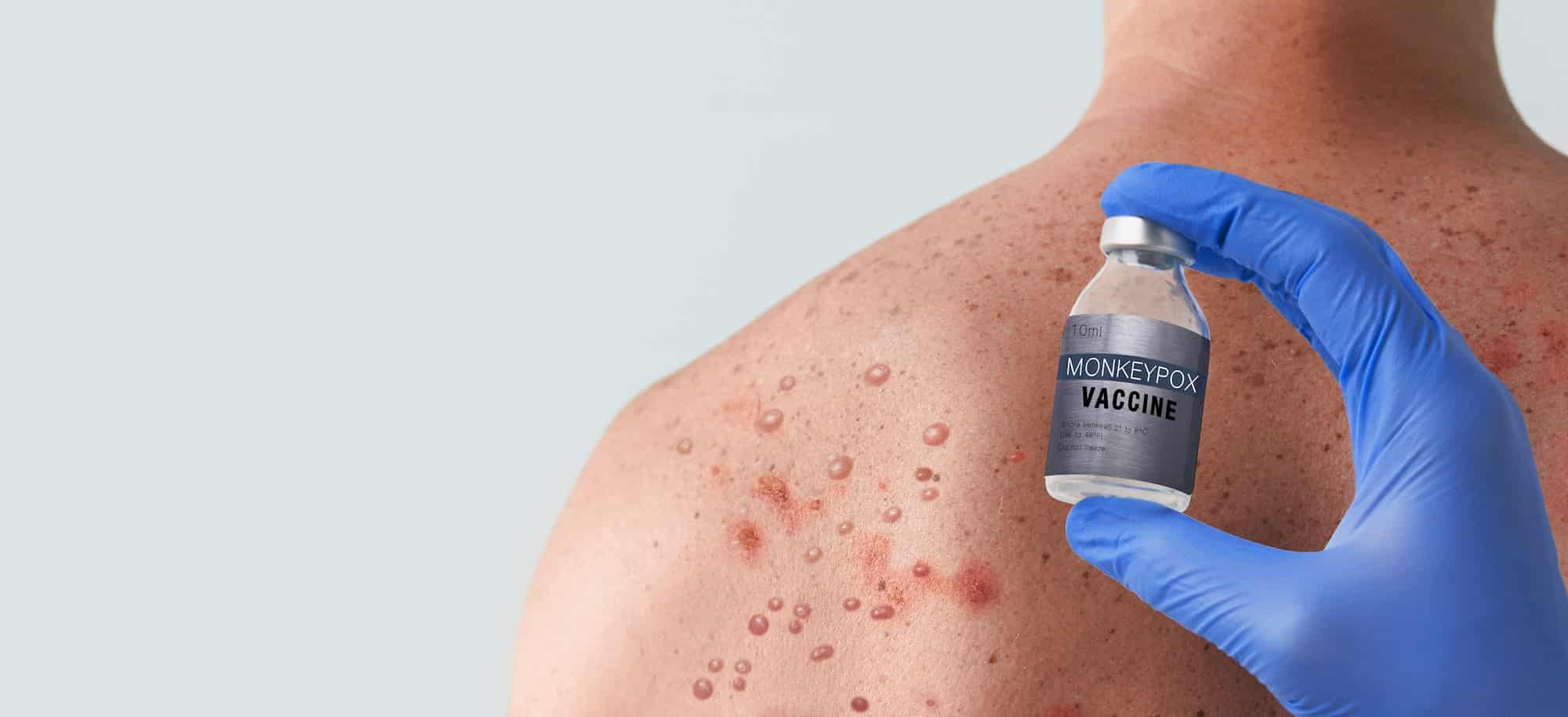
Symptoms of mpox includes lymph node swelling, fever, headache, back and muscle pain, weakness, and almost all have a skin rash. The rash starts in the center of the body and spreads outward and can be seen on the palms and soles. The rash lasts 14-28 days and most people recover without treatment.
In more serious cases, it can lead to eye infection and blindness, problems with the nervous system, inflammation of the heart and complications (skin infection) of the mouth, rectum, and genital lesions. Treatment is available if the infection becomes severe called Tecovirimat (TPOXX) that is being used in ongoing clinical trials. The initial trial in DRC in 2020 shows the medication does not stop the symptoms but can decrease the chance of dying by half from 3.6 % to 1.7 %.
How is mpox spread?
Mpox is spread by person-to-person skin contact, kissing, sex, direct contact with infected animals (monkeys, squirrels, and rodents), contact with contaminated materials including bedding, and in pregnant women can spread to the fetus.
In cases found outside of Africa, it disproportionally affects gay and bisexual men. The virus has been detected in lesions and also in semen. The risk to the general population in the United States is very low but the best way to prevent infection is to avoid high risk activity and to get vaccinated if part of a group at risk.
Interestingly, in 2023 in Spain there was a reported outbreak of mpox in a body piercing and tattoo parlor where 36 % of its patrons were infected with the virus. In this outbreak there was no sexual activity reported. The lesions and pustules (pus fill fluid) appeared within 7 days near the area of piercing or tattoo.
Who should be vaccinated for mpox?
Best way to protect yourself is to avoid high risk activity, and in the United States (U.S.) if part of a high-risk group including men who have sex with men (MSM), men with multiple sexual partners, or sex workers consider vaccination. This is protective against both the weaker and more deadly strain.
In the U.S., 1 in 4 of high-risk persons have been vaccinated. The vaccination (JYNNEOS) in a 2022 study showed that one dose has 36 % protection and two doses up to 66 %.
Where did mpox come from?
Mpox or monkey pox was discovered in 1958 in Copenhagen in a colony of monkeys kept for research. It was then reported in rodents and monkeys and transmitted to people.
The first human case was in DRC in 1970 and in 2022 spread around the world. It was renamed mpox to follow modern guidelines of naming and also into different strains including clade I and II.
Who gets mpox?
In most people, symptoms resolve however people at risk include:
(1) those with weakened immunity like people with advance HIV, (2) close contacts with people with rashes or body fluid infected with mpox, (3) people with eczema or skin conditions as pox virus can penetrate the skin easier, (4) children less than age of 1, (5) pregnant women, and (6) high risk populations including sex workers, and men who have sex with men (MSM).
What should I do if infected with mpox?
Immediately seek medical help and go to the emergency room. They can put you on the appropriate precautions and test for the virus and treat with medication if needed. If you test positive your case will be reported to the Center for Disease Control (CDC) and they will work closely with your doctor to be sure you receive the proper care.
CDC continues to monitor the sewage in the U.S. for signs of outbreak.



 Have Questions? AskDoctorH
Have Questions? AskDoctorH